




Did you find this useful? Give us your feedback








4 citations
25 citations
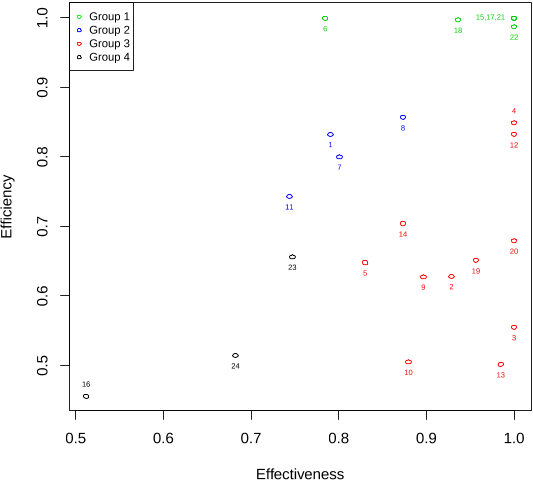
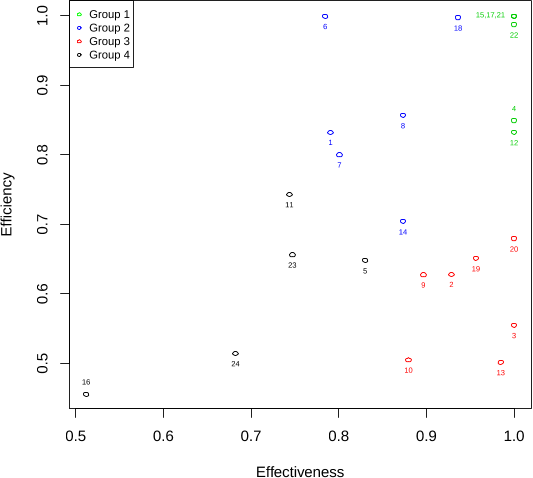
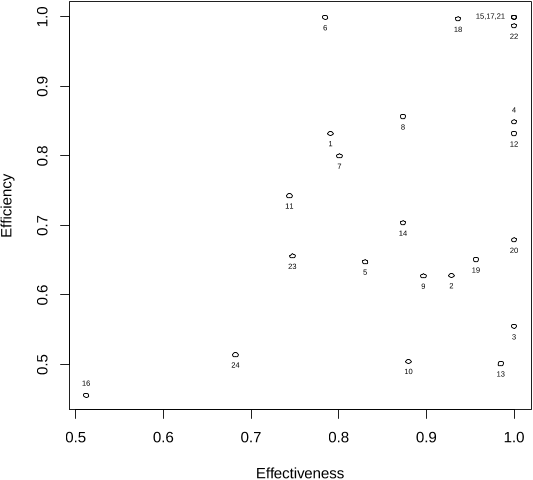
...While performance evaluation of hospitals has been explored in prior literature (Zheng et al. 2018, Castelli et al. 2015, Varabyova and Schreyogg 2013, Hollingsworth 2008), the performance of physicians has proven to be more difficult to assess because of diversity in patient mix and treatments,…...
[...]
25 citations
...…is considered to be more effective if the chance of returning to the ED (e.g., due to an unresolved issue) is minimized per hour spent in the ED.1 Both the LOS and 72-hour rate of return metrics have been used in the literature as valid measures (see, e.g., Chilingerian 1995, Fiallos et al. 2017)....
[...]
24 citations
...Saghafian et al. (2018) study the speed-quality tradeoffs in a telemedical physician triage system in the context of an ED setting....
[...]
23 citations
...…a high 72-hour return rate is an undesirable indicator of care delivery effectiveness in the ED (see, e.g., Abualenain et al. 2013, Pham et al. 2011, Klasco et al. 2015), we use the proportion of patients discharged by a physician who did not return to the ED within 72 hours of their original…...
[...]
...The 72-hour rate of return has also been proposed as a measure of quality in the Emergency Medicine literature (see, e.g., Abualenain et al. 2013, Pham et al. 2011, Klasco et al. 2015) although using it for measuring quality (which is different than effectiveness) of care is controversial....
[...]
12 citations
...Collier et al. (2006) use the total billable charges attributed to physicians as one of the outputs of their proposed model....
[...]