




Did you find this useful? Give us your feedback








4 citations
150 citations
149 citations
...…to his/her cognitive abilities, his/her 1 In EDs, the service is provided by a specific physician who is in charge of the patient, and the ED service is very rarely composed of a teamwork among physicians (see, e.g., Saghafian et al. 2012, Saghafian et al. 2019, and the references therein)....
[...]
140 citations
...Specifically, given the large body of literature examining the effects of high workloads on physician performance (KC and Terwiesch 2009, Powell et al. 2012, Berry Jaeker and Tucker 2017, Batt and Terwiesch 2017), we study whether and how physician effectiveness and efficiency are affected by high ED volume....
[...]
...…given the large body of literature examining the effects of high workloads on physician performance (KC and Terwiesch 2009, Powell et al. 2012, Berry Jaeker and Tucker 2017, Batt and Terwiesch 2017), we study whether and how physician effectiveness and efficiency are affected by high ED volume....
[...]
138 citations
...…given the large body of literature examining the effects of high workloads on physician performance (KC and Terwiesch 2009, Powell et al. 2012, Berry Jaeker and Tucker 2017, Batt and Terwiesch 2017), we study whether and how physician effectiveness and efficiency are affected by high ED volume....
[...]
123 citations
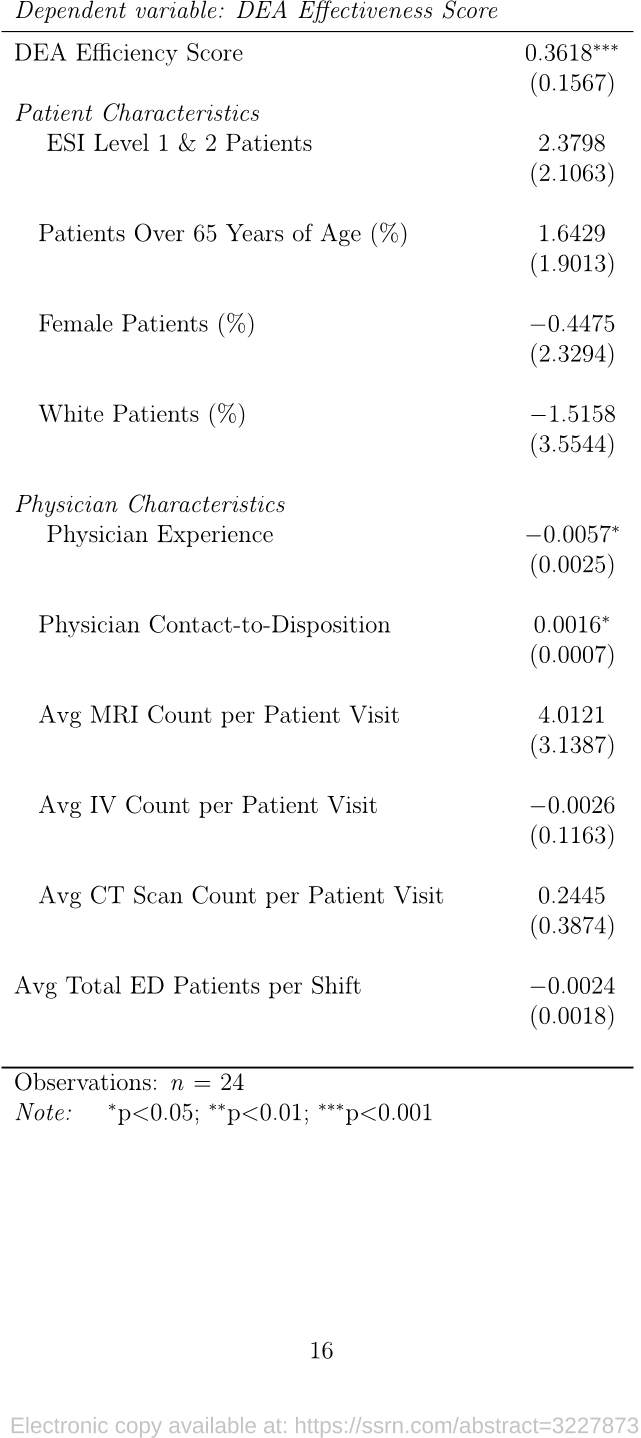
...Low-ESI patients and those older than 65 are known to be patients that have a relatively higher contact-to-disposition time than other patients (Latham and Ackroyd-Stolarz 2014)....
[...]